Estradiol is the main, active estrogen in the body. It is important for female and male sexual health and reproduction. It also helps with brain and thyroid function, as well as with bone and skin health. In this post, we’ll walk you through the function effects of estrogen produced in the body.
Disclaimer: This post covers the science and health effects of estrogen that’s naturally produced in the body – it’s not about estrogen (estradiol) medication. Estradiol, as part of hormonal therapy, needs to be prescribed by a doctor. Please discuss your medications with your doctor.
What Is Estradiol?
Definition
Estradiol is a sex hormone and steroid. Estradiol-17β (E2) is the most active estrogen in the body. It is produced mainly in the ovary, but the brain, fat tissue, immune cells, and bones can also produce estradiol [1].
It is produced from testosterone and progesterone, which are also sex hormones [1].
In the brain, P-450 aromatase enzymes are responsible for its formation. Studies indicate that estradiol levels are highest at birth, and gradually decline as we age [2].
Normal Levels
In the blood, estradiol exists in 2 forms. It is either bound to proteins (SHBG or albumin) or is unbound (free). It is difficult to measure or predict free estradiol levels, and thus, most estradiol measurements only measure bound estradiol [3].
Estradiol levels in healthy, menstruating women range from 25 to 500 pg/mL. Normal levels may vary from lab to lab. Levels are also affected by the phase of the menstrual cycle [4]:
Sometimes, doctors may use estradiol levels for ovarian reserve testing (a fertility test) because this helps check follicular activity. Although it is fast and inexpensive, it is never used alone as a marker for ovarian reserve because many factors can increase estradiol [5].
In postmenopausal women, levels below 6.0−55 pg/mL are usually considered normal.
The normal range in men is typically 7.6−42.6 pg/mL.
Estradiol and other estrogen levels can be measured through both blood tests and urine tests. Blood tests are more common [6].
Some lab-to-lab variability occurs due to differences in equipment, techniques, and chemicals used. Don’t panic if your result is slightly out of range–as long as it’s in the normal range based on the laboratory that did the testing, your value is normal.
However, it’s important to remember that a normal test doesn’t mean a particular medical condition is absent. Your doctor will interpret your results in conjunction with your medical history and other test results.
Have in mind that a single test isn’t enough to make a diagnosis. Your doctor will interpret this test, taking into account your medical history and other tests. A result that is slightly low/high may not be of medical significance, as this test often varies from day to day and from person to person.
Function of Estradiol
1) Sexual Development & Reproduction
In Women
Estradiol is important for female development since it is the main source of estrogen. It drives the development of secondary sex characteristics (breasts, widened hips, etc.) from birth to puberty [7, 8].
It also affects the brain and behavioral differences between males and females [2].
Estradiol controls gonadotropin-releasing hormone (GnRH) secretion [9].
During the menstrual cycle, estradiol helps increase hormones (luteinizing hormone) that induce ovulation [9].
Estradiol also plays a role in pregnancy. At normal levels, it helps maintain pregnancy. But at high levels, estradiol reduces fertility. A combination of synthetic estradiol and progesterone is used in birth control pills to prevent ovulation and pregnancy [10].
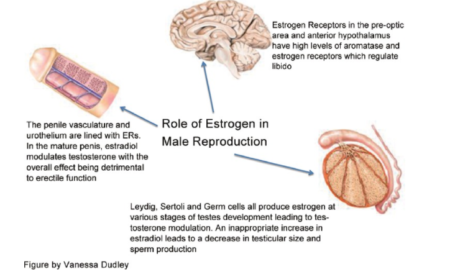
In Men
Males also need estradiol for their sexual development and function as it helps with erectile function, sperm formation, and sexual libido. However, its exact roles are still unknown [11].
Scientists are investigating whether stimulating estradiol receptors can help prevent cell death (apoptosis) in penis tissues [11].
On the other hand, too much estradiol may decrease sex drive. Also, high estradiol and low testosterone may cause breast development in men and other issues due to hormonal imbalance [11].
2) Bone Development & Maintenance
Estrogen is needed for adequate bone growth and the maintenance of bones and joints [12].
Post-menopausal women with both early and late forms of osteoporosis have estrogen deficiency. Estrogen deficiency also contributes to the development of osteoporosis in elderly men [13].
Scientists think that estrogen may act by reducing the activity of bone-degrading cells (osteoclasts), which may help maintain bone mass and strength [14].
3) Brain Function
Estradiol can reach the brain, where it helps protect brain structure and function. It’s hypothesized to have neuroprotective effects in the cerebral cortex, hippocampus, basal forebrain, and striatum [15, 16].
Limited research suggests that estradiol may play a role in the creation of connections between nerve cells in the brain; it seems to inhibit or promote this process depending on the location within the brain. It might also influence the physiology of developing nerves in the brain [15].
Researchers posit that estradiol may be, in part, responsible for gender differences in brain function – including thinking, stress, anxiety, aggression, and movement [2].
Estradiol also promotes or prevents cell death (apoptosis) in some parts of the developing brain, which contributes to sex differences. For this reason, large doses of estradiol can also be toxic [15].
Neuroscientists think estradiol can increase dopamine, which may affect motivation (especially sexual motivation). It might also affect cognition [17].
In a study of 31 males and 39 females, women with higher estradiol levels performed better on memory tasks than women with low estradiol. The high estradiol group was also more accurate than the males [18].
A review suggested that post-menopausal women who have lower estradiol may perform worse on verbal memory and fluency tasks than pre-menopausal women [19].
However, in another study of 16 healthy women, estradiol levels were not associated with brain function, memory, or learning. Large-scale studies are needed [20].
Animal studies suggest that estradiol may enhance brain function, but the potential mechanisms and how they relate to humans are still unclear [16, 21].
In other animal experiments, a lack of estrogen may have contributed to the decline in brain function in older female rats when compared to older male mice [22, 23].
Some researchers believe that estradiol helps protect against cortisol‘s negative effects on the brain, but this hasn’t been proven in large-scale studies. This is simply based on the observation that post-menopausal women who have lower estrogen levels seem to be more susceptible to stress and have worse brain function in response to stress. But a cause-and-effect relationship hasn’t been established [17].
4) Weight
Science suggests that estradiol plays a role in controlling appetite, energy usage, body weight, and fat distribution in women. Exactly how estrogen does this and what it means for the average woman looking to keep her weight under check is still an area of research [9].
For example, scientists found that estradiol helps control CCK, a hormone implicated in satiety and digestion. Limited human studies suggested that estradiol might affect meal size and fullness [24].
Another observation is that post-menopausal women with lower estrogen levels gained weight, but those who had hormone therapy did not. However, many factors beyond estrogen are likely at play [24].
Additionally, estradiol in the blood may affect feelings of fullness (satiety) via the hypothalamic-pituitary-gonadal (HPG) axis, which is involved in eating behavior [24].
In female rats, the lack of estradiol in the blood and a dysfunctional HPG axis led rats to overeat and become obese. This link hasn’t been confirmed in humans [24].
5) Thyroid Health
Estrogen seems to have both direct and indirect effects on thyroid health. For one, we know that two types of estrogen receptors are found in thyroid tissues: ERα and ERβ. These receptors appear to have slightly different roles, where ERα may promote thyroid cell formation and growth [25].
Some studies suggest that thyroid diseases and thyroid cancer are more common in women, which made scientists wonder whether estrogen plays a role in thyroid diseases. So far, the findings have been inconclusive.
In rats, low estrogen levels caused the thyroid to underperform. Meanwhile, high estrogen levels led to hyperactivity in the thyroid [26].
Human studies are needed.
6) Skin Health
Researchers think that estrogen may play a big role in skin health, though its exact effects are still elusive. There are many estrogen receptors on the skin. By acting on these receptors, estrogen might impact skin strength, thickness, and even hair growth [27].
Estrogen may also help with wound healing, but more human data are needed. In one review, lower estrogen levels were linked with excessive inflammation and delayed wound healing [28].
Interestingly, limited studies found that some women had improved psoriasis during their pregnancy. Scientists are debating whether elevated during estradiol played a role, since their psoriasis worsened after giving birth. However, the levels of many other hormones change during pregnancy, and estrogen may not be the most important one [29, 30, 31].
During menopause, the skin becomes more wrinkled and loses some of its strength and firmness. Skin collagen, which provides support for the skin, also declines during menopause [32, 33].
Reduced estrogen levels in rats (caused by ovary removal) also cause the skin to age quicker [34, 35].
However, the effects of topical estrogen – as creams, lotions, and gels – on skin health in women hasn’t been established. According to one review, topical estradiol may help improve skin collagen levels, reduced wrinkling, improved skin moisture, and helped heal wounds and scars. Its safety and efficacy in humans have yet to be determined [33].
Remember, estrogen is only available with a doctor’s prescription for certain medical indications. It’s not approved for cosmetic purposes.
7) Heart Health
After menopause, women’s estradiol levels may decrease by around 75 to 90%.
Some scientists hypothesize that increased age and low estrogen levels contribute to heart disease. However, scientific data are lacking to back them up. The existing evidence on estrogen deficiency increases and heart disease risk is controversial and the results have been mixed [36].
One review suggested a link between premature menopause and early heart disease. Als, women with ovarian failure have a higher rate of heart disease [36].
However, these studies dealt with associations only. A cause-and-effect relationship hasn’t been established.
Limited prospective studies suggested a potential protective effect of hormone therapy against heart disease, but other studies showed the opposite [36].
Some studies didn’t find any effect. For example, a single-blinded study of 2,700 women found that estrogen therapy did not reduce heart disease rates [37].
Additionally, during menopause, women are more likely to develop metabolic syndrome (high blood sugar, high blood pressure, high cholesterol, weight gain). Metabolic syndrome plays a big role in heart disease risk, but the impact of estrogen deficiency on metabolic syndrome is poorly understood [38].
High-quality, large-scale human studies are needed.
Does Estradiol Have Any Negative Effects?
Naturally-produced Estrogen vs. Medication
Naturally-produced estrogen is not thought to have any negative effects, especially at normal levels.
The potential risks mentioned below mostly dealt with synthetic estrogen therapy. Some studies looked at bioidentical estrogen, though these are less common.
For example, menopausal hormone therapy (MHT) can effectively reduce symptoms of menopause. It consists of estrogen and progestins to compensate for their declining levels in women with an intact uterus [39].
MHT may help with hot flashes, mood swings, insomnia, night sweats, vaginal dryness, and restlessness. Various combinations of natural or synthetic estrogens or progestins can be used, which are all linked to different health risks and benefits [40].
Many of the below-discussed findings are considered controversial, and experts agree that more research is needed to understand the long-term impact of hormone therapy.
Cardiovascular & Cancer Risks
Understanding the Research
Most of the claims about the increased risk of breast cancer span from misinterpreting cellular, animal, and human studies on premenopausal women. Additional misinterpretation spans from assuming synthetic and natural are the same [41].
As an example of misinterpreting non-human studies, estrogen was found to activate certain cancer-causing genes (BRCA1, BRCA2, etc.), which hypothetically increase the risk of breast cancer and endometrial cancer in cell culture. Other genes are thought to be involved in estrogen formation and certain pathways (CYP17, CYP19, and HSD17B1) [42, 43, 44].
These studies are early experiments in test tubes. They help scientists understand certain pathways or chemical structures in the body, but they don’t tell us anything about the actual risk of estrogen in animals or humans.
Synthetic vs. Natural Estrogens After Menopause
When it comes to misinterpreting human data, synthetic and natural estrogens are often looked at together, though their risks likely differ.
Synthetic estrogens (conjugated equine estrogens) and synthetic progestins (medroxyprogesterone acetate) have been associated with an increased risk of breast cancer, especially when compared only to synthetic estrogens [39].
A study of data collected over 50 years showed that synthetic estradiol+progestogen therapy in post-menopausal women was associated with an increase in breast cancer 3 years after the therapy [45].
In contrast, natural progesterone and estrogen did not increase breast cancer risk in large observational studies. These were carried out in France and included over 100k women who were followed up for 6 – 9 years [41, 39, 40].
Other studies looked at stroke risk.
In a 6-year study of 16,000 post-menopausal women, the group of women who took 0.625 mg of synthetic estrogen plus progestin daily had a higher risk of stroke than the group who only took a placebo. The women were generally healthy and had no other risk factors, indicating that typical postmenopausal hormone therapy may increase stroke risk [46, 47].
However, in a review, researchers showed that the increase in stroke risk after hormone therapy was rare. Large-scale, multi-center trials are required to understand the risks better [48].
FDA Warnings About Hormone Therapy
According to the FDA, women should not take hormone therapy for menopause if they [49]:
- Think they are pregnant,
- Have problems with vaginal bleeding,
- Have had certain kinds of cancers,
- Have had a stroke or heart attack,
- Have had blood clots,
- Have liver disease.
The FDA also mentions that Menopause Hormone Therapy (MHT) may increase risks of serious side effects including blood clots, heart attacks, strokes, breast cancer, and gallbladder disease in some women [49].
If you’re considering MHT, it’s important to talk with your healthcare provider. They will outline all the potential risks and benefits of this therapy in your case.
In Men
Men are physiologically supposed to have lower estrogen levels than women. And unlikely in women, levels in men usually stay approximately the same throughout life.
High levels of estradiol in men have been linked with an increased risk of prostate cancer, but n definitive association can be drawn at this point. More data are needed.
Various studies had conflicting results. Some conclude that estrogen is associated with a higher risk for prostate cancer due to changes in genes and increases in inflammatory markers (IL-1β, IL-6, iNOS, etc.) [50].
Estradiol can increase prolactin levels, which is also associated with higher breast and prostate cancer risk [50].
In rats, treatment with estrogen and testosterone increased their chances of prostate cancer development [51, 52].