Multiple sclerosis (MS) is the most common autoimmune disease of the nerves. It has gained notoriety over the years affecting celebrities such as Montel Williams, Richard Pryor, and Jamie-Lynn Sigler. Read on to discover the causes, diagnosis, mechanisms, and risk factors of MS.
What is Multiple Sclerosis?
Multiple sclerosis (MS) is a chronic autoimmune debilitating disease in which nerve damage (demyelination of neurons) in the brain and spinal cord disrupts their communication with the body.
MS is a leading cause of disability in young adults and is the most common inflammatory disorder of the brain. It’s most common in young women, but other groups can be affected, too [1].

Diagnosis and Symptoms of MS
Demyelination and damage to neuronal axons can lead to many observable negative health effects and symptoms associated with multiple sclerosis. Clinical diagnosis can be made through medical imaging (MRI) and laboratory testing (CSF testing) [2].
While MS symptoms vary greatly from patient to patient, these commonly include [3, 2, 4, 5, 6]:
- Painful eye movement and blurred vision (damage to the optic nerve)
- Tremors and loss of coordination/balance (damage to the cerebellum)
- Limb and muscle weakness, spasms, and numbness lead to mobility problems (damage to the spinal cord)
- Electric-shock sensations provoked by neck movements (Lhermitte sign)
- Blurred or double vision (damage to the brainstem)
- Constipation, incontinence, bladder problems, or erectile dysfunction (loss of upper motor neuron control)
- Speech impairment and trouble swallowing; however, only a small percent of MS patients are affected by these symptoms (impairment of motor speech processes in the brainstem)
- Memory and cognitive problems
- Fatigue, which may potentially coexist with depression
- Depression: MS is strongly correlated with depression – up to 41.8% of MS patients has clinical depressive symptoms
Given that MS patients display different symptoms unique to themselves, the management should be tailored to the patient and each symptom mitigated individually. Patients facing fatigue and muscle weakness can undergo physical therapy to be able to undertake daily activities [7].
Based solely on these symptoms, MS is difficult to diagnose non-invasively because the disease shares many symptoms with other neurological disorders such as acute disseminated encephalomyelitis and neuromyelitis optica. As a result, clinical symptoms combined with medical imaging/laboratory testing, known as the McDonald diagnostic criteria, are sufficient for the diagnosis [8, 9].
Understanding how your DNA and lifestyle factors influence your risk for multiple sclerosis (MS) can offer valuable insights into your overall health. By analyzing these factors, you can gain a clearer picture of your likelihood of developing MS. With SelfDecode’s Longevity Screener, you can explore how your genetics and lifestyle combine to affect your risk, helping you take proactive steps to support your long-term health.
Progression of Multiple Sclerosis
When MS first develops, typically in younger patients (teenage-30 years old) it often presents as relapse-remitting MS – the disease flares up and then disappears. After 1-2 decades, it can progress into secondary progressive MS, when the symptoms don’t go into remission and may progressively get worse. This pathway is observed in about 85% of the cases [10].
The remaining 15% of MS cases are primary progressive MS, which starts as progressive. In some cases, the disease can be initially progressive and then go into remission [11].
Early Warning Signs
Damage to the axons of neurons is an early event and continues over time. Surprisingly, the severity and degree of the damage decrease over time [12, 13].
Due to the damage to neuronal axons, the signs and symptoms of the early stages of MS are very similar to those of the later stages, which include [14, 3]:
- Vision loss or pain in the eyes (optic neuritis)
- Blurred vision (brainstem syndromes)
- Numbness or tingling in limbs (brainstem and spinal cord syndromes)
- Mobility problems (dysfunction of long tracts)
Risk Factors and Potential Exacerbating Causes of MS
The causes and risk factors of MS are still not fully understood. It is a complex disease with many varying and interconnecting factors affecting its development and onset. Both environmental and genetic factors together contribute to MS [15].
1) Gender and Sex Hormones
Women are twice as likely to develop MS than men [16, 17].
In women, the onset of MS is generally earlier. However, men tend to progress faster and have a more severe disease course [18].
This disparity is potentially caused by differences in sex hormones and the immune environments between men and women [18].
Hormones and MS
Immune cells have receptors for hormones, and they affect immune function.
Estrogen may enhance autoimmunity at low levels. However, at higher concentrations, it has the opposite effect – it protects against MS by shifting from inflammatory Th1 to Th2 [18].
This might explain why MS and several other Th1-dominant autoimmune diseases improve during pregnancy, since estrogen level increases during pregnancy [19].
On the other hand, prolactin and growth hormones, which are also higher in women, enhance autoimmunity [18].
2) Age and Race
MS can strike at any age but people between 16-55 are at a higher risk. Additionally, white people of European descent are more likely to develop MS compared with other races [20].
3) Viral Infections
There are two general hypotheses for the infectious causes of MS, both involving a widespread microbe rather than a rare pathogen [21].
According to the hygiene hypothesis, viruses can increase the risk of developing MS if acquired in late childhood or during adulthood. However, acquiring the virus before would produce protective immunity in the individual [21].
One common virus that is associated with MS is the Epstein-Barr virus, which causes mononucleosis. Similar latent viruses might also be causal agents of MS [22, 23].
Despite finding a positive correlation, studies have not identified a single infectious pathogen as the causative factor for MS [24].
4) Vitamin D Deficiency and Lack of Sun Exposure
This hypothesis is supported by the environmental risk factor for vitamin D deficiency. Increasing exposure to sunlight and increasing vitamin D levels are correlated with decreased MS risks. This correlation is supported by epidemiological evidence that MS frequencies are more prevalent in high latitudes, where sunlight is of lower intensity [23, 25].
5) Cigarette Smoking
Cigarette smoke:
- Increases oxidative stress [26]
- Contain neurotoxic substances [27]
- May alter immune function and cause brain inflammation [28, 26]
Therefore, smoking not only increases the risks of MS but also accelerates the progression from relapsing-remitting to secondary progressive MS [29, 30].
In addition, cigarette smoking can increase the risk of other immune-related diseases [31].
6) Other Autoimmune Diseases
People with other autoimmune conditions, such as type 1 diabetes or IBD, have a slightly higher risk of developing MS [20].
7) Other
The following factors might also contribute to MS development, but the available research is inconclusive.
Stress
For stress and MS, the most compelling factors include [32]:
- Stressor duration: Long-term stressors have contributed to MS relapses [33]
- The severity of the stressor: Intermediate to strong intensity stressors are more strongly associated with MS relapses [33]
- The frequency of the stressor: Accumulation of stress increases the risk of MS relapses [32]
- Cardiovascular reactivity and heart rate: Higher heart rate and cardiovascular responses to stressors will increase the risk of relapses [33]
- Social support: A stronger social support and network can reduce relapses associated with MS [34]
Dietary Factors
The results of dietary studies and risks of MS need to be interpreted with caution as most of them are observational. Such studies are prone to confounding factors or bias and typically do not imply causation without additional evidence.
Saturated Fat and Polyunsaturated Fats
There is one study observing participants over a long period on the effects of dietary fat and the risks of developing MS. In this study, neither animal nor saturated fats were associated with an increased risk for MS [35, 36].
Low consumption of plant-based foods and high consumption of animal products correlated with higher MS rates in one smaller study [37].
Higher omega-3 fatty acid (alpha-linolenic, but not EPA or DHA) intake may reduce the risk of MS [38].
Dietary Antioxidants
Lower vitamin C and juice intake, but not intake of vitamin E, beta-carotene, or fruits and vegetables increased the risk of MS [39].
Other studies did not find any significant association between vitamins C, E, or fruits and vegetable intake and the risks of MS, but the potential benefits of these nutrients and antioxidants cannot be excluded [40, 41, 42, 36].
Obesity
Higher body mass index may be associated with higher MS rates [39].
Dairy Products
Consumption of milk, rather than cheese, may correlate with an increased risk of MS [43].
A milk protein called butyrophilin has some similarities to a myelin protein called myelin oligodendrocyte glycoprotein. If the body develops an antibody against this protein, this can lead to MS. In a rat model of MS, butyrophilin can trigger MS-like symptoms [44, 45].
Adjuvants
Vaccine adjuvants are immune-stimulating agents that are typically contained in vaccines to increase the immune response to the antigen in the vaccine. They can be microbial products such as LPS-like substances, mineral salts, metals like aluminum and thimerosal (mercury), emulsions, microparticles, and liposomes [46].
How adjuvants make vaccines work better is not completely understood. Generally, the adjuvants stimulate the immune system, including inflammatory immune responses. Vaccines that are made to raise an immune response against bacteria and viruses typically trigger cellular (Th1) immunity [47].
In multiple cases described in scientific literature, vaccine adjuvants may contribute to autoimmune responses [47, 47].
In MS patients, some experts recommend using vaccines without adjuvants to avoid over-stimulating the immune system [48].
That said, the connection between adjuvant use and MS rates has not been firmly established and requires further investigation.
Toxic Chemical Exposure
Most studies that look at occupational toxic exposures and MS risk focused on organic solvents [24].
In an Italian study, people who worked in the shoe and leather industry had a higher prevalence ratio of MS, ~5x higher compared to other people [49].
Many other studies have shown that occupational chemical exposures somewhat increase the risk of developing MS. However, all of these cases were based on prevalent cases (those who already developed the disease) and do not directly prove cause and effect.
Potential Mechanisms of Nerve Damage in MS
It’s important to note that the mechanisms behind the nerve damage in MS are still being researched, and it’s too early for drawing definite conclusions. The proposed mechanisms below are suggested by preliminary studies but shouldn’t be taken for granted until more research is done.
The hallmark of MS is the formation of [50]:
- Lesions in the nervous system
- Sclerotic plaques
- Inflammation
- Demyelination of neurons in the brain
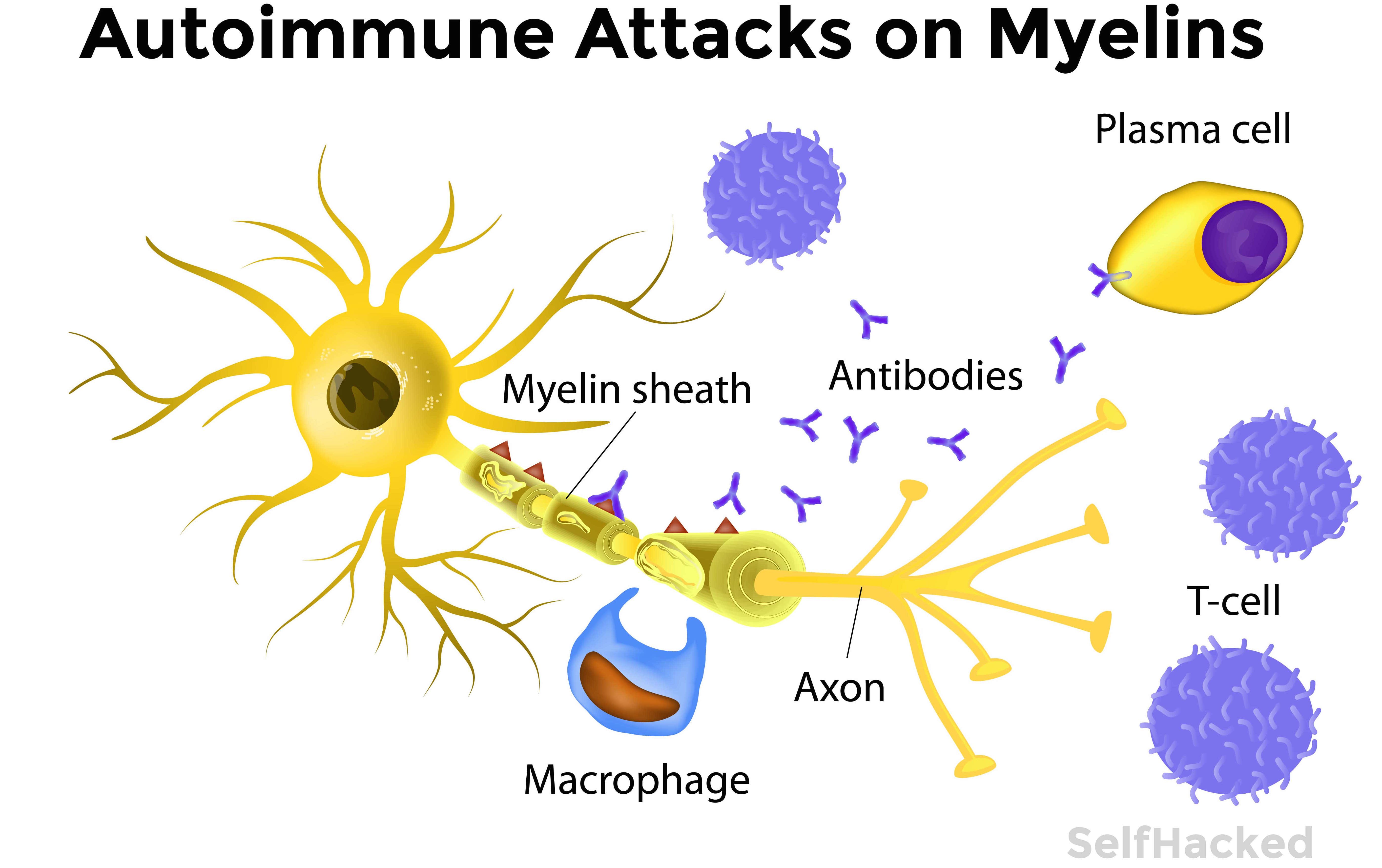
The myelin sheath is a white, fatty, and electrically insulating substance surrounding the axons of neurons. It allows for faster conduction of electrical impulses.
Proteins on myelin, such as myelin basic protein and proteolipid protein, can be attacked by myelin-reactive T cells, which are typically present in the blood of healthy people, but not activated [51, 52].
When they are activated and there is a leaky blood-brain barrier, T cells can cross it and attack the myelin sheaths in the brain [17].
How Myelin-Reactive T Cells Are Activated
Myelin proteins, including myelin basic protein and proteolipid protein, have some amino acid similarities to viruses, bacteria, and food components.
When the immune system is activated by the following pathogens or foods, it can trigger MS. However, other factors, such as overall inflammation levels, blood-brain barrier permeability, and imbalanced immune system may be at play [53, 54].
These triggers can’t cause MS on their own but may contribute to its development, along with other factors.
Pathogens [17]:
- Epstein-Barr Virus
- Herpes Virus
- Papilloma Virus
- Various bacteria including Pseudomonas
The gut bacteria Bacteroides thetaiotaomicron and Bacillus fragilis typically don’t cause diseases, but they have proteins that are similar to the myelin proteins. These gut bacteria could potentially trigger multiple sclerosis [55].
Milk or dairy products contain the protein butyrophilin, which has some similarities with the proteins on myelin sheaths [44].
Imbalanced Immune System (Th1, Th2, and Th17)
White blood cells of MS patients have abnormal inflammatory responses in all three Th systems (also called T-helper cells or CD4+ T cells), including [56]:
- Increased Th1 cytokines (IFN-gamma)
- Increased Th2 cytokines (IL-4 and IL-5)
- Increased Th17 cytokines, including IL-17
- Increased TNF-alpha
- Decreased anti-inflammatory cytokines (IL-10)
- Decreased regulatory T cells (the cell that prevents inflammatory Th1, Th2, and Th17 from autoimmune or allergic responses) [57]
In addition, the levels of IL-17 and IL-5 correlated with the number of active plaques on MRI images [56].
CD4+ T cells are T helper cells that release cytokines that help suppress or regulate immune responses and are present in acute MS lesions [58].
Intestinal Permeability or “Leaky Gut”
“Leaky gut” or increased gut permeability may be a precipitating factor in autoimmune diseases by allowing inflammatory components to leak into the bloodstream and over-activate the immune system [59, 60].
Recent studies have suggested the connection between “leaky gut” and MS prevalence and severity, once again confirming the importance of the gut-brain axis [61, 62].
In 124 MS patients, increased intestinal permeability correlated with disease severity and progression [63].
In a small pilot study, more patients with relapsing-remitting MS had increased intestinal permeability (73%) compared to healthy controls (25%) [64].
On the other hand, inflammation of the (central) nervous system can also increase gut permeability and affect the structure of the small intestine mucosa, so it’s a vicious cycle [65].
While the emerging research promises to answer some questions about the mechanisms behind MS, it’s too early for drawing definite conclusions.
Gut Microbiota
According to preliminary research, microbial imbalance and maladaptation in the gut (gut dysbiosis) may play a role in the development of autoimmune diseases [66].
An altered physiology of gut mucosa and microbiota can affect intestinal permeability, allowing the passage of different macromolecules (from foods), toxins, and bacteria, which may trigger MS [64].
The gut bacteria can also influence the blood-brain barrier integrity [67].
The gut microbiota plays an important role in educating the immune system. T cells (regulatory and helper) become more knowledgeable of the composition of cells and chemicals in the gut [68].
On the other hand, the disease can also lead to dysbiosis [69].
MS patients have a reduced number of gut bacteria species and an imbalance of certain bacterial families compared to healthy people [70, 71, 69].
However, despite the role of gut microbiome in autoimmunity, further studies are needed to identify the specific microbes that can potentially induce an autoimmune reaction by the T cells [68].
A Leaky Blood-Brain Barrier
The function of the blood-brain barrier is to protect the brain preventing foreign and unnecessary materials to reach the brain, like errant T cells [72].
Autoimmunity and inflammation can damage this barrier potentially contributing to a leaky blood-brain barrier (BBB). On the other hand, an impaired BBB allows toxins and inflammatory cells to enter the brain and inflict further damage, so it’s another vicious cycle [73, 53].
In normal circumstances, errant cells undergo induced cell death (apoptosis) by external body signals. The rogue T cells in MS are unresponsive to these signals, so they accumulate in the brain and spinal cord forming plaques and causing inflammation [50].
In MS, the inflammation is caused by myelin-reactive T cells, which destroy the myelin sheath. Demyelination can lead to irreversible damages to the axons and MS progression [74].
Moreover, recent studies have demonstrated that B cells from MS patients are also capable of directing immune responses against neurons (neural antigens) [75].
Oxidative Stress
Plaque formation and lesions may be caused by oxidative stress and mitochondrial injury [76].
Oxidative stress plays an important role in the progression of MS. Reactive oxygen species (ROS) contribute (act as mediators) to demyelination and axonal damage in the brain [77].
Due to the low concentration of antioxidants in the brain, reactive oxygen species are effective at causing oxidative damage to the cells in the brain and the whole nervous system [78].
Oxidative stress can lead to inflammation, while inflammation can also cause oxidative stress. Through a self-perpetuating process, these two contribute to the progression of MS [79].
Learn More
- Multiple Sclerosis: Diets and Complementary Approaches
- Multiple Sclerosis: Genes, Epidemiology & Prevention
Find Out More About Inflammation
For more information on autoimmunity causes, treatment, and complementary approaches, check out the course All About Inflammation.







