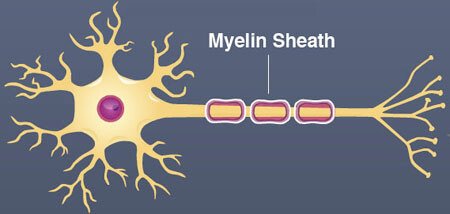
Myelin is an important part of the nervous system and is vital for optimal cognitive function. This article will walk you through the science behind natural factors that may increase myelin in the body.
What is Myelin?
Overview
The myelin sheath is a protective cover made out of fats and proteins that wraps around the axons (projection) of nerve cells. It insulates neurons so they can send electrical signals faster and more efficiently. This supports brain health and nervous system function [1, 2].
Factors that May Increase Myelination
When to see a doctor
If your goal is to increase myelin to improve your neurological issues–including those of cognitive dysfunction – it’s important to talk to your doctor, especially your symptoms are significantly impacting your daily life.
Your doctor should diagnose and treat the condition causing your symptoms.
Additionally, brain structure is not something that people can change on their own with the approaches listed below. Instead, the factors listed here are meant to support overall brain health, nutrient balance, and well-being.
However, the impact of most of the factors listed below on myelination have not been studied in humans.
Therefore, you may try the additional strategies listed below if you and your doctor determine that they could be appropriate.
Read through the approaches listed here and discuss them with your doctor before trying them out. None of these strategies should ever be done in place of what your doctor recommends or prescribes.
Lifestyle Choices
1) Sleep
Animal studies suggest that sleep increases the amount of oligodendrocyte precursor cells (OPCs) in the body, which can lead to increased myelin formation. Sleep has been associated with higher expression of genes coding for myelination [3].
Researchers found that the production rate of the myelin-making cells (oligodendrocytes), doubled as mice slept [3].
The increase was most marked during the type of sleep that is associated with dreaming (REM sleep) [3].
In contrast, the genes involved in cell death and stress responses were turned on when the mice were forced to stay awake [3].
Getting enough restful sleep is good for overall brain health and well-being. Human studies are needed to examine the effects of sleep on myelination.
2) Exercise
Animal research suggests that exercise may increase myelin after an injury and in mouse models of Alzheimer’s [4, 5].
Exercise also seems to increase mitochondrial function, which increases myelin, in animals fed a high-fat diet [6].
We still don’t know how exercise impacts myelin in humans, but we do know that regular exercise supports brain health [7].
3) Socializing and New Experiences
Limited research suggests that socializing and enriched environments may support myelination, especially during early development.
The number of myelin-forming oligodendrocytes increased 27 to 33% in the visual cortex of rats raised in environments that are enriched by additional play objects and social interaction [8].
Enriched environments increased the number of myelinated axons in the corpus callosum of monkeys and rats [8].
Early experience increased white matter structure in human infants (internal capsule and frontal lobes) in parallel with improved performance in behavioral tests [8].
Children suffering from severe childhood neglect have a 17% reduction in the corpus callosum area [8].
4) Learning New Complex Skills
Learning complex skills, such as playing the piano, are accompanied by increased white matter in brain areas involved in musical performance [9].
White matter increased proportionately to the number of hours each subject had practiced the instrument, indicating white matter increases when acquiring certain skills [9].
Nutrition/Dietary Factors
1) Fish/DHA (Brain)
DHA is deposited within the cerebral cortex at an accelerated rate during the last trimester of pregnancy and during the first 2 years after birth [10].
This early accelerated rate of DHA deposition coincides with the onset of myelination, a process that is sensitive to DHA accumulation and stores [11, 12].
A reduction of DHA in the diet negatively affects DHA concentrations within the brain [13, 14, 15].
Animal models suggest that the consequences of dietary DHA deficiency may be a high omega-6 to omega-3 ratio in brain fatty acid composition and deficiencies in learning and memory [16, 17].
Researchers think this might be due, in part, to negative impacts on neurite outgrowth and myelination [18].
More clinical data are needed.
2) Vitamin D
Maintaining normal vitamin D levels supports bone health and immunity. Animal studies show that vitamin D3 may induce functional recovery and increased myelination in a rat model of facial nerve injury. Scientists are researching whether the vitamin D receptor can increase the production of oligodendrocytes. Human studies are required [19, 20].
3) Vitamin C
According to animal studies, vitamin C may help with myelin formation [21].
Vitamin C, also known as ascorbate, is important as a cofactor in several enzyme reactions. Scientists suspect that ascorbate-dependent collagen synthesis may help with myelination. Ascorbate added to rat Schwann cells and neurons promoted myelin formation [22].
Human studies are lacking.
4) Iodine
Iodine is essential for many bodily functions. Animal research suggests that iodine deficiency may impair myelination. Supplementation with iodine helps improve myelin formation in nerve cells, but no clinical data back up this finding [23].
5) Zinc
Some researchers believe that zinc is needed for myelin proteins to function correctly. Zinc deficiency may cause problems with myelin formation and defective sheaths [24].
6) Choline and Lecithin
In animal models of multiple sclerosis, the choline pathway seems to help with remyelination of myelin sheaths. It enhances myelin repair. This pathway hasn’t been investigated in people with MS [25].
CDP-choline improved myelination in animal models of multiple sclerosis [26].
After drug-induced demyelination, CDP-choline enhanced myelin regeneration and reversed motor coordination deficits [26].
The increased remyelination arose from an increase in the numbers of proliferating oligodendrocytes and oligodendrocyte precursor cells [26].
Lecithin is a component of myelin [27].
The effects of these compounds on myelination in humans have yet to be researched.
7) Vitamin B12
Vitamin B12 deficiency can cause demyelination and problems with early brain development. Therefore, adequate vitamin B12 intake may help with sheath formation [28].
8) Iron
Iron plays a key role in proper cell function. Some studies suggest that normal iron levels are needed for myelin formation. Iron deficiency has been linked with poor myelination. Therefore, iron may support myelination in the body (oligodendrocytes), but more human data are needed [29].
9) Vitamin K
Myelin membranes are particularly enriched with glycolipids, including galactosylceramide (GalCer) and its sulfated form, sulfatide [30].
Animal findings suggest that concentrations of sulfatides increase during brain development, parallel to an increase in brain myelination [30].
Decreases in myelin sulfatides content and/or changes in their molecule structure have been implicated as important factors in the disruption of myelin structure, with subsequent attenuation of myelin efficiency as an axonal insulator [30].
Decreases in the content of myelin sulfatides with age have been implicated in behavioral deficits observed in normal aging, and age-associated neurological disorders. However, no large-scale human studies have confirmed this link [30].
Theoretically, getting adequate amounts of vitamin K may support myelination. Vitamin K has been implicated in increasing sulfatides; a link between sulfatides and vitamin K has been suggested. In the brain, vitamin K is mostly found as vitamin K2 or menaquinone-4 (MK-4) [30].
Human data are needed.
10) Biotin
Some scientists consider that biotin activates enzymes involved in energy production and myelin synthesis [31].
In one small study, about 91.3% of people with multiple sclerosis (MS) improved clinically with high doses of biotin. An improvement was delayed from 2 to 8 months following treatment onset [31, 31].
Two multi-centric double-blind placebo-controlled trials are currently underway. We have yet to see if their results will support the use of biotin in MS or not [31].
11) Folate/Vitamin B9 (Brain)
Folate deficiency during pregnancy caused lower myelination in rat offspring. Getting enough folate is especially important in the first trimester, during which the nervous system forms. However, myelination happens later in the baby’s development. Exactly how it is affected by prenatal folate intake remains to be determined [32, 33].
12) Pantothenic Acid/Vitamin B5
Pantothenic acid might indirectly help with myelin formation by supporting fatty acid synthesis (myelin is rich in lipids) [34].
Chickens deficient in pantothenic acid developed skin irritation, feather abnormalities, and spinal nerve damage associated with the degeneration of the myelin sheath [34].
Human data are lacking.
13) Copper
Copper might be important for myelination (oligodendrocytes), but clinical trials are needed to confirm this. When animals are given a drug that binds to copper, demyelination results [35].
14) Phosphatidylserine
Some studies described interactions among phosphatidylserine, cognitive activity, cognitive aging, and retention of cognitive functioning ability. There are insufficient data to draw conclusions on the effects of phosphatidylserine on myelin in humans, though [36].
Early research suggests that phosphatidylserine is required for healthy nerve cell membranes and myelin [36].
Additionally, the aging of the human brain has been associated with biochemical alterations and structural deterioration that impair neurotransmission [36].
Supplemental phosphatidylserine (300 to 800 mg/d) seems to be absorbed well in humans and likely crosses the blood-brain barrier. Scientists are investigating whether it slows, halts, or reverses biochemical alterations and structural deterioration in nerve cells [36].
According to some scientists, this compound may support human cognitive function: short-term memory formation, long-term memory consolidation. It’s also been hypothesized to affect the ability to create new memories, retrieve existing memories, learn and recall information, focus attention, reason and solve problems, and communicate verbally [36].
Further clinical trials are required.
15) Thiamine
Vitamin B1 may help with the development of the myelin sheath, according to research in thiamine-deficient rats. Scientists think it is required both by the nerve cells and by other supporting cells in the nervous system [37, 38].
This B vitamin is being researched in neurodegenerative diseases such as Parkinson’s, Alzheimer’s, and Huntington’s disease [39].
16) Keto Diets
The impact of keto diets on myelination is still unclear and proper clinical trials are lacking. Carefully consult your doctor before switching to a keto-type diet.
Some scientists have proposed that ketones (3-hydroxybutyrate) may help support myelin growth by being a source of energy and fuel for lipids [40].
The ketogenic diet might improve myelination by compensating for a certain enzyme (AGC1, which helps make N-acetylaspartate in oligodendrocytes) that causes seizures and poor development in people who lack this enzyme. Much more research is needed to see if ketogenic diets are beneficial for people with this rare type of genetic disorder [41].
17) Cholesterol
Cholesterol is an essential constituent of myelin. The dry mass of myelin is about 70 to 85% lipids. Cholesterol is needed for myelin membrane growth. Its presence is needed in the membranes in order for the sheath to function normally [42].
And although cholesterol is harmful in excess, clinical trials should examine whether getting sufficient amounts from nutritious foods like eggs, sardines, or yogurt may be healthy and good for myelination. But be sure to talk to your doctor before increasing your intake of high-cholesterol foods.
Supplements
Make sure to speak with your doctor before taking any supplements. Let them know about any prescription or over-the-counter medication you may be taking, including vitamins and herbal supplements.
If you and your doctor agree that supplementing is a good idea, choose products made by a trusted and reliable manufacturer.
Remember that dietary supplements have not been approved by the FDA for medical use. Supplements generally lack solid clinical research. Regulations set manufacturing standards for them but don’t guarantee that they’re safe or effective.
Evidence is lacking to recommend any of the supplements listed below for myelination. Early animal or cellular research has explored whether the following supplements increase myelin:
1) Gotu Kola
Gotu kola helps rats make a more rapid functional recovery and a greater number of myelinated axons following nerve damage [43].
2) Uridine
Uridine may reduce myelin sheath lesions in animals [44].
3) Ashwagandha
Ashwagandha has an active component called withanoside IV. In mice, withanoside IV increased myelin levels [45].
4) SAMe and Methylation
S-adenosylmethionine (SAMe) helps regulate DNA methylation. DNA methylation plays a key role in myelin development. Scientists are investigating whether SAMe can increase myelination in neurons [46].
Folate and B12 deficiency during pregnancy also cause lower myelination in rat offspring [32, 33].
5) Myoinositol
Chronic low blood sodium levels may cause the destruction of myelin. Myoinositol seemed to reduce myelin loss and normalize blood sodium levels in animals [47].
6) Ozone
Ozone improved facial nerve health and resulted in thicker myelin sheaths in rats [48].
7) Grape Seed Extract (Body)
In diabetic rats, grape seed extract protected against demyelination (Schwann cells) [49].
8) Lion’s Mane
The mushroom lion’s mane (Hericium erinaceus extract) quickened the process of myelination in animals and promoted normal development of myelin sheaths [50].
9) Ginkgo (Body)
After an injury, Ginkgo increased myelination in animals and Schwann cells [51].
10) Supplemental Lithium
Some researchers are exploring if lithium can help increase myelin (via its GSK3b inhibitory effect) [52].
Treatment of adult mice with lithium after facial nerve crush injury stimulated the expression of myelin genes, restored the myelin structure, and accelerated the recovery of whisker movements [52].
Lithium also promoted remyelination of the sciatic nerve after crush [52].
The effects of regular and low-dose lithium on myelination in humans are unknown. Clinical trials are needed.
Other
Scientists are investigating whether:
- PQQ increases myelin in Schwann cells [53].
- Quercetin increases myelin-producing cells (oligodendrocytes) after injury [54].
- The antioxidant flavonoids luteolin, quercetin, and fisetin can reduce the amount of myelin macrophages break down (phagocytosis) [55]
The impact of these compounds on myelination hasn’t been explored in animals or humans.
Other Factors & Pathways that May Increase Myelin
This section summarizes the science behind hormonal, cellular, and drug-related factors that may increase myelin. Our aim is to discuss the research findings.
Do not take any of the below-mentioned substances without talking to your doctor.
Some of the substances listed here can have detrimental health effects if used inappropriately. Be sure to discuss all your medications, supplements, and lab results with your doctor.
1) Melatonin
In rats that had a stroke, melatonin helps promote myelination. It decreased white matter inflammation and increased myelination in nerve cells [56].
2) Progesterone
Progesterone can promote the formation, repair, and regeneration of myelin sheaths in animal models [57, 58, 59].
Progesterone is available only by a doctor’s prescription. It is indicated only for specific hormonal disorders in women.
The delivery of natural progesterone, however, represents a challenge because of its metabolism in the digestive tract and liver [59].
Recently, the intranasal route of progesterone administration has received research attention for easy and efficient targeting of the brain. Clinical trials need to further explore these formulations [59].
Progesterone in the brain is derived from glands or from local synthesis by neural cells. Stimulating the natural formation of progesterone is currently explored as an alternative strategy for neuroprotection, axonal regeneration, and myelin repair [59].
3) IGF-1
Insulin-like growth factor-1 (IGF-1) has been identified as a growth factor that promotes myelination by stimulating the early events of myelination in Schwann cells and oligodendrocytes [60].
IGF-1 stimulates 2 key fatty acid synthesizing enzymes via the PI3K/Akt signaling pathway [61, 62].
4) Thyroid Hormones
Scientists are investigating whether triiodothyronine (T3) stimulates myelin protein genes and remyelination in the adult brain by making myelin cells (oligodendrocytes) mature faster [63, 64].
5) Testosterone
Estimates suggest that men are less likely to develop multiple sclerosis than women [65].
According to limited research, testosterone stimulates the formation of new myelin and reverses myelin damage in chronically demyelinated brain lesions (oligodendrocytes, working via the androgen receptor) in animals [65].
Clinical trials (phase II) have found treatment with testosterone can increase gray matter in males with multiple sclerosis. However, its effect on white matter-where myelin is located — hasn’t been explored [66].
6) Prolactin
Prolactin during pregnancy is necessary for the increase of myelin [67].
7) VIP
Animal research suggests that VIP (and PACAP) may contribute to the myelinating process, including myelin maturation and synthesis, and help regulate the expression of myelin proteins [68].
8) Erythropoietin
Researchers are studying if erythropoietin (EPO) induces the expression of myelin genes in oligodendrocytes. These genes have been linked with neuron repair, possibly by inducing remyelination after myelin damage. However, this only happens in the erythropoietic EPO receptor (EPOR)-expressing CG4 cells [69].
9) Acetylcholine and Acetylcholinesterase Inhibitors
Cholinergic treatments, such as acetylcholinesterase inhibitors (AChEIs), may have beneficial effects on myelination, myelin repair, and myelin integrity [70].
Increasing cholinergic stimulation helps the myelination process [70].
Cholinergic treatments, such as nicotine, huperzine A, and galantamine could help promote myelination during development and myelin repair in older age [70].
The acetylcholine muscarinic receptors may increase the survival of precursor cells that increase myelin [71].
10) Brain-Derived Neurotrophic Factor
The neurotrophin brain-derived neurotrophic factor (BDNF) helps regulate myelin formation in the nervous system. An increase of BDNF levels has been linked with an increase in the rate of myelination in animal and cellular studies. Scientists think this causes an increase in myelin content and thickness [72].
11) Nerve growth factor
Some researchers posit that nerve growth factor (NGF) may help repair myelin damage. It may also induces the production of another substance that can help increase myelination [73].
Cellular research is investigating whether NGF promotes axonal regeneration, survival, protection, and production of oligodendrocytes and facilitates their migration to the sites of myelin damage [73].
12) CB1 Cannabinoid Receptor
The CB1 cannabinoid receptor, which is activated by naturally-produced cannabinoids, is being researched for increasing myelin formation in oligodendrocytes (via mTOR and AKT) [74].
13) GSK3b Inhibitors
GSK3b inhibits myelin-dependent axon outgrowth; in theory, inhibition of GSK3b may increase myelin [75].
According to some poorly-researched theories, GSK3β inhibition stimulates the regeneration of myelin-forming cells and remyelination following chemically induced demyelination (oligodendrocytes) [76].
14) N-acetylaspartate
N-acetylaspartate (NAA) may supply acetyl groups for myelin synthesis. Some researchers think it’s needed for the formation and maintenance of myelin.
15) RXRgamma
A protein called retinoid X receptor gamma (RXRgamma) seems to promote oligodendrocyte precursor cells [77].
RXRgamma must combine with the Vitamin D Receptor to induce gene expression and create these myelin-producing cells [77].
No animal or human data are available.
16) PPAR-delta and PPAR-gamma
PPAR-delta is a protein that has been linked with energy expenditure and weight loss. Some theories suggest it also causes myelin cells to multiply, but human data are lacking [78].
PPAR-gamma is a protein that may have anti-inflammatory effects. Studies are investigating whether it promotes myelin formation and growth (oligodendrocyte) [79].
A variety of factors might increase/decrease their function.
17) Neuregulin 1
NRG1 is a protein that helps increase Schwann cells. Scientists think neuregulin 1 is important for synaptic plasticity, inhibiting the amygdala (to shut down anxiety), myelination (Schwann cell maturation, survival, and motility), and heart function (cardiac growth factor). Human studies are needed [80].
18) GDNF
Glial cell line-derived neurotrophic factor (GDNF) seems to be capable of increasing axonal regeneration myelin in cells, but its effects in animals and humans are unknown [81].
19) Pregnenolone
We don’t know how pregnenolone might affect myelination in animals or humans. Pregnenolone is considered an unapproved drug by the FDA. We highly recommend against taking it.
Pregnenolone is a neurosteroid produced in the body. According to some theories, these brain-produced hormones known as neurosteroids may regulate the synthesis and repair of myelin. This theory has not been verified, though.
Pregnenolone is a precursor of other steroid hormones. Research on Schwann cells is studying if natural increases in pregnenolone can raise myelin formation [82].
Others
Epidermal Growth Factor Receptor (EGFR) and ErbB3 receptor tyrosine kinase:
- Epidermal growth factor receptor plays an important role in myelination and remyelination. EGFR signaling hypothetically increases myelin repair and myelination [83].
- ErbB3 receptor tyrosine kinase is a receptor located on Schwann cells. Inhibition of its expression may, theoretically,l result in reduced myelination [84].
Factors that May Reduce Myelination
There’s not enough reliable information about factors that may reduce myelination. Most of the studies outlined below deal with associations or were conducted in animals or cells. Human data are lacking.
We’re outlining the following factors to present research findings only.
If you’re worried about myelination, talk to your doctor to get accurate diagnosis, treatment, and recommendations on complementary brain-healthy habits that you can incorporate into your daily routine.
1) Inflammation
It’s thought that inflammatory cytokines reduce myelination [85].
Myelin and oligodendrocyte (OL) destruction occur in cultured preparations subjected to cytokines such as TNF alpha and lymphotoxin (LT) [85].
Multiple sclerosis is a disease that causes demyelination. Some studies have shown these and other cytokines to be elevated at lesion sites and in the Cerebrospinal fluid of multiple sclerosis (MS) patients, with similar findings in animal models. More human studies are needed [85].
2) Alcohol
Teen binge drinking is associated with low frontal white matter integrity [86].
In rats, adolescent binge drinking reduced the size of the corpus callosum, and degraded myelin basic protein in the gray matter [86].
Myelin was also damaged on axons in the prefrontal cortex (medial) in adolescent rats who binge drank – and heavier drinking predicted worse performance on the working memory task in adulthood [86].
These findings establish a causal role of voluntary alcohol on myelin and give insight into specific prefrontal axons that are both sensitive to alcohol and could contribute to the behavioral and cognitive impairments associated with early-onset drinking and alcoholism [86].
3) Statins
Statins are drugs that help treat heart disease. Some controversial animal studies suggest that statins may have a negative impact on oligodendrocytes and myelin formation. Large-scale human data is needed to verify these claims [87].
4) EMF Exposure
One study concludes that EMFs from things like cell phones and Wi-Fi can cause myelin deterioration. Human data are lacking [88].
5-6) SIRT1 and AMPK Activation
SIRT1 and AMPK activation are thought to be normally good, but when it comes to myelin, scientists suggest they might not be great.
SIRT1 inactivation increases the production of oligodendrocytes (myelin-producing cells). In mice, SIRT1 inactivation will lead to oligodendrocyte production, which then increases the formation of myelin and white matter abnormalities [89].
Likewise, when AMPK levels are high in animals, myelin production is slowed [90].
Human research should explore these links.
Limitation and Caveats
There are many different models that are cited when we say that a certain factor may increase or decrease myelin. As mentioned, the studies brought down do not provide enough evidence to make a conclusion that they will increase myelin in humans.
The article is simply listing these as potential contenders for increasing myelin in humans.This post is to be used as a springboard for you to to do further research.
Takeaway
The myelin sheath wraps around brain cells, enabling them to send out signals at high speed. It supports brain health and cognition throughout the lifetime.
However, strategies that might improve myelination mostly rely on data from small-scale human studies or animal experiments.
Some healthy ways to potentially enhance myelination include getting enough sleep, exercise, sunlight, and learning new skills. Making sure your diet contains plenty of DHA, B vitamins, and choline might also help.
Lastly, it’s a good idea to avoid unhealthy habits like heavy drinking and constant cell phone exposure — these seem to disrupt myelin in experimental studies.
