The MTHFR gene is very important for DNA production & many bodily functions. Read on to discover the science behind MTHFR and folate metabolism, plus how to check your SNPs.
What is MTHFR?
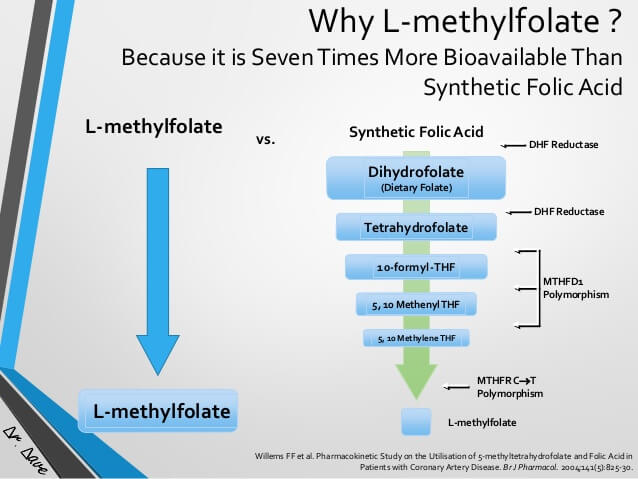
The MTHFR gene codes for an enzyme known as methylenetetrahydrofolate reductase or MTHFR. This enzyme is responsible for converting 5, 10-methylene THF to 5-methyl THF, which is essential for the conversion of the amino acid homocysteine to methionine [1, 2].
This enzyme is very important for the production of DNA and methylation pathways that are essential for all bodily functions [2].
MTHFR also plays a central role in the transformation of folate to S-adenosylmethionine (SAM), the universal methyl donor in cells and affects DNA methylation status.
To learn more about methylation in general, check out this post.
The Two Main MTHFR SNPs
Genetic variations in the MTHFR gene results in reduced activity of the enzyme produced and have been associated with a series of diseases and conditions, including cardiovascular disorders, neurological defects, some forms of cancer, psychiatric disorders, diabetes, and pregnancy complications [3, 4].
The two most common MTHFR mutations (polymorphisms) found in humans are:
- MTHFR C677T (Rs1801133). This mutation (the A allele) is associated with reduced enzyme activity, elevated total homocysteine levels and altered distribution of folate [1]. People with an “A” allele for this mutation present a 35% decrease of the normal enzyme activity and “AA” individuals a 70% decrease [5].
- MTHFR A1298C (rs1801131). This mutation also impacts MTHFR enzyme activity and homocysteine levels but to a lesser extent than C677T [1].
The enzymatic activity of MTHFR in people with one minor allele in each MTHFR C677T and A1298C polymorphisms is lower than the activity present if only one SNP had a single minor allele [6].
Reduced MTHFR enzyme activity results in a decreased conversion of the amino acid homocysteine to methionine and accumulation of homocysteine in the blood. Abnormally elevated homocysteine levels are referred to as “homocystinuria” or “hyperhomocysteinemia” (Hhcy) [4].
The elevation of homocysteine levels in the blood may increase susceptibility to a number of health conditions [3, 4].
A series of studies have linked MTHFR polymorphisms, especially the C677T, with various types of diseases, but the results are sometimes conflicting and controversial. This controversy may be attributed to small sample sizes and ethnic factors that impact on the presentation of diseases in different populations around the world [2].
The various diseases that have been associated with MTHFR polymorphisms, especially C677T, are briefly presented below.
Conditions Linked to MTHFR C677T Mutations
An association between a given genotype and a condition or disease doesn’t necessarily mean that genotype causes that disease. That being said, the A allele at the C677T polymorphism has been associated with many health conditions, including:
- Strokes of various kinds in different populations [7, 8, 9, 10] and stroke in children [11]
- Heart disease if lower folate levels [12]
- High blood pressure (also GG of MTHFR A1298C) [13]
- Male infertility especially in Asian populations (homozygous AA) [14, 15, 16, 17]
- Depression [18] – high Homocysteine and dysfunction of methylation metabolic pathways are critical to the synthesis of noradrenaline and serotonin [19].
- Autism spectrum disorders [20, 21, 22, 23]
- Alzheimer’s [24, 25]
- Dementia [26]
- Parkinson’s [24, 25]
- Multiple sclerosis, though the evidence in controversial [27, 28, 29]
- Rheumatoid Arthritis [30]
- ADHD (A1298C) [31]
- Migraines with or without aura [32, 33, 34] – A different study found that the “AA” genotype was inversely associated with migraines. However, those with the “AA” genotype who did have migraines also had heart problems significantly more often [35].
- Diabetes and diabetic kidney problems (nephropathy) in patients with type II diabetes. The risks vary between Caucasian, Asian, Arabic and Chinese Han populations [36, 37, 38, 39].
- Schizophrenia [40, 41]
- Unipolar depressive disorder and bipolar disorder [40, 41]
- Cancer: It has been previously demonstrated that folate deficiency can increase the incidences of different forms of cancer. MTHFR is directly involved in folate metabolism and therefore MTHFR mutations may have an impact on the development of cancer [2, 42].
- Prostate cancer [2, 42]
- Ovarian cancer [2, 42]
- Esophageal cancer [2, 42]
- Stomach cancer [2, 42]: people with the “A” allele were more likely to develop stomach cancer after an H Pylori infection [43].
- Bladder cancer [2, 42]
- Brain cancer [44]
- Lung cancer [45]
- Kidney cancer [46]
- Head and neck cancer [47]
- Colon cancer & and more side effects from 5-fluorouracil treatment [48]
- Hearing impairment [49]
- Lower Bone Mineral Density in the spine and neck [50]
- Cluster Headache [51]
- Epilepsy [52]
- Peripheral Arterial Disease [53]
- Worse outcomes for end-stage kidney disease [54]
- Adverse effects of methotrexate in rheumatoid arthritis [55] and Increased liver toxicity from methotrexate (folate blocker) [56]
- Recurrent pregnancy loss [57, 58]
- Pre-eclampsia, a serious complication of pregnancy [59].
- Having a child with Down’s syndrome (if the mother has one or both “A” alleles) [60]
- Neuronal tube defects (NTD) such as anencephaly and spina bifida in newborns [61]
- Cleft lip and palate [62]
- Lower luteinizing hormone (LH) [63]
- Cataracts [64]
- Alopecia Areata [65]
- More severe colitis [66]
Again, it’s important to take these associations with a grain of salt until more robust studies investigate them further. If you have a genotype linked to low MTHFR activity and you’re concerned about any particular health condition, your doctor can help you develop an appropriate strategy for prevention.
Testing Homocysteine and Folate
It should be noted that most of the studies done on MTHFR genes only show correlations with disease when homocysteine levels are high or folate levels are low. You may therefore want to ask your doctor about testing for folate or homocysteine. High homocysteine levels show that you may have a methylation issue or a B12/ folate deficiency caused by a possible MTHFR mutation.
If your tests show high homocysteine, your doctor will likely advise you on an appropriate diet and supplement regimen. This plan is likely to include an increased intake of folate, vitamin B12 (cobalamin) and vitamin B6 (pyridoxal phosphate), which have been found to affect the levels of homocysteine in the blood [4].
A vitamin-rich diet that includes fruits, vegetables, dark leafy greens (spinach, kale, bok choy, and Swiss chard), eggs and red meat provide the B vitamins needed to maintain low homocysteine levels. Additionally, supplementation with all three vitamins, folate, B12, and B6 can normalize homocysteine levels [4].
The healthy control group had homocysteine under 7 μmol/l, whereas those with schizophrenia averaged 12 μmol/l [67].
Checking Your MTHFR SNPs
MTHFR is an enzyme which affects the methylation of all cells. Methylation is important for various biochemical conversions which determine the expression of your genes [2].
For MTHFR C677T:
- Each A allele has been associated with lower methylation activity and higher homocysteine [2]
- AA = 60 – 70% reduced MTHFR enzyme activity
- AG = 30 – 40% reduced enzyme activity, respectively, as determined by in vitro analysis of the MTHFR activity [68, 69, 70].
In other words, those with one copy of the “A” allele were found to have a MTHFR enzyme about 60-70% as effective as those without the “A” allele. Those with two copies of the “A” allele (the “AA” genotype) were found to have a MTHFR enzyme only 30-40% as effective as those without the “A” allele.
Check the SNPs out on SelfDecode:
Bioavailable vs Synthetic Folates
It has recently been shown that the human gut can convert the folates from food sources to 5-MTHF (the type of folate that our body can use) very efficiently. However, its ability to convert supplemented folate is limited [71].
Reduced folate ((6S) 5-MTHF) is the bioavailable form of folate which is easily absorbed and metabolized in the human body. It is available as a supplement, usually labeled as methylfolate or L-methyltetrahydrofolate [72, 73, 74].
Additionally, you can supplement with methyl-vitamin B12 (methylcobalamin), the bioavailable form of vitamin B12, instead of the usual vitamin B12. This will make access to vitamin B12 for your body easier.
If you are homozygous for both of the best-known MTHFR mutations (rs1801133 “AA” and rs1801131 “GG”), we strongly recommend talking to a doctor about supplementation and other options.
Buying Folate

Folate is an important micronutrient in DNA synthesis, integrity, and stability. If you have alleles that reduce the activity of MTHFR, we recommend looking for the active methylfolate (or L-methyltetrahydrofolate) variety. Talk to your doctor before starting a new supplement to make sure it’s right for you.
Folate Requirements
The current recommended intake is 400 μg/day for the average adult with an increase to 600 μg/day for pregnant and lactating women [4].
Keep in mind that folate supplementation is known to mask anemia caused by insufficient levels of vitamin B12. To avoid a B12 deficiency, keep your medical professional in the loop about any supplements you choose to take [75].




